Hypophysis Gland TÜMÖROS
More Common in Women
Pituitary tümörs are more common in women, just like endocrine thyroid disease.
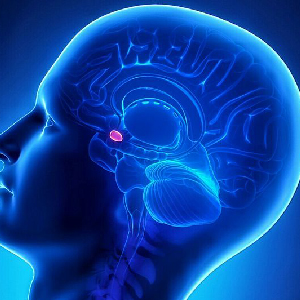
Hypophysis Gland
What does it do?
Which hormones does it regulate?
How does it affect hormones when it becomes cancerous?
What is done in treatment?
What happens after surgery?
Pituitary gland tümörü, the exact cause of which is unknown, is one of the multidisciplinary topics of medicine. These masses, which are rare and usually benign, cause many different complaints by affecting our hormones produced by the pituitary gland.
Don't be fooled by its small size (5-7 mm). Located at the base of the skull, behind the nasal bridge, the pituitary gland is a hormone gland with more important functions than its size would suggest. It secretes different hormones according to the needs of our daily functions in our body's states such as night-night, wakefulness and sleep; not only that, it also manages hormones that enable us to grow over a long period of time, such as growth, heart rate, thyroid gland secretions, and hormones that enable us to move. Like an orchestra conductor, the thyroid gland regulates the functioning of other endocrine glands, such as the glands of the kidneys, the testes in men and the ovaries in women. As a result of the uncontrolled growth and enlargement of the cells that make up the tissue of this gland for various reasons, some masses called "pituitary adenoma" are formed. Although pituitary adenomas are generally benign in terms of their function and structure, they can adversely affect health with various clinical symptoms depending on their size and function.
In the diagnosis and treatment of pituitary gland tümörs, in addition to neurosurgery, endocrinology and radiation oncology are also important actors in the multidisciplinary process.
What are some of the symptoms?"
Pituitary gland tümörs can have different symptoms depending on the hormone that affects the tümörür. But in general, you can review the list of symptoms below:
- Headache
- Gör vision disorders
- Menstrual period changes, delays
- Infertility
- Breastfeeding (except during pregnancy)
- Cushing's syndrome caused by excess ACTH (adrenocorticotropic hormone) production
- Acromegaly caused by excessive production of the growth hormone acromegaly (growth of the hands, feet, and neck)
- Fatigue without cause
- Psychological problems
“Pituitary tümörs, which bring together different disciplines in the diagnosis and treatment process, are not escaping from the current health technologies. Especially in cases with large tümörüs, we operate our patients in hybrid operating room conditions using navigation technology. In this way, we can pinpoint the exact location of the tümörün, reducing the risk of possible injury and error.”
Görevs of our hormones
Growth hormone (GH): It affects the entire body, allowing the organs to mature and grow during the growth and development period.
Adrenocorticotropin hormone (ACTH): It regulates the production of vital hormones such as cortisol, aldosterone and androgens, which are secreted by the muscle glands. It also protects our body against stress.
Thyroid stimulating hormone (TSH): Another vital group of hormones for the vücut, T3-T4 regulates the production of thyroid hormones.
Folic & follicular stimulating hormone (FSH): In women, it is responsible for the development of ovarian follicles. In men, it is involved in regulating the production of sperm. It is also responsible for regulating the production of sex hormones such as estrogen, progesterone and testosterone.
Lüteinizing hormone (LH): In women, it is responsible for the release of maturing egg cells into the reproductive tract, while in men it is responsible for sperm production and maturation. It is also involved in the regulation of the production of sex hormones together with FSH.
How to recognize it
According to scientific findings, there is no known cause for pituitary gland tümörs. Although trauma, severe births, thyroid problems, radiation or certain immunotherapy drugs can affect the pituitary gland's functioning, none of these can cause tü'mö's. A large proportion are hormonally inactive and some are detected by chance. Diagnosis is made by looking at the hormones in the pituitary gland and examinations consisting of several stages. The clinical symptoms of these structures, which are rarely seen, basically vary depending on the pituitary pituitary gland from which they originate, whether or not they produce hormones and the tümör size they reach. In other words, in fact, symptoms specific to which hormone it affects can be observed. It is easier to recognize in women because it can be detected in prolactin (the hormone that ensures the production of breast milk) levels. In men, the problem is usually detected after the tümör has grown a little bigger.
“The aim of surgical treatment is to establish a pathological diagnosis, to remove compression of all nerves and vessels, to control abnormal hormone activity and to preserve as much normal pituitary tissue as possible.”
Adenomas smaller than 1 cm in diameter are called microadenomas, while adenomas larger than 1 cm are called macroadenomas. Although microadenomas often do not cause any significant problems in the surrounding tissues, macroadenomas cause problems in the anatomical structures in the pituitary gland and by compressing the pituitary gland. In addition, adenomas can produce certain hormones in excess of normal amounts, uncontrollably, depending on the hücre from which they originate. Accordingly, adenomas that can reject growth hormone, ACTH, TSH, prolactin, FSH or LH hormones can develop. Tümör structures (such as craniopharyngioma, teratoma, gangliocytoma), which are located in or around the pituitary gland and originate from different tissue types from the embryological period in the womb, can also develop.
MUST SEEK A DOCTOR IF YOU HAVE COMPLAINTS
Due to the mass effect of the Tümörün, symptoms such as headache, visual field disorders, blurred vision, and drooping of the eyelid may occur, while different symptoms may occur in cases of excessive or insufficient secretion of hormones. For example, over-secretion of the growth hormone causes hand and foot, and even body growth in adults. When TSH (Thyroid Stimulating Hormone) is over-secreted, heart diseases, weight loss and thinning of the skin are encountered. Excessive secretion of the hormone ACTH (Adrenocorticotropic Hormone) can cause many different complaints, including Cushing's disease, brittle bone disease, weight gain in the waistline or abnormal hair growth. Or let's talk about the excess secretion of the hormone prolactin, which ensures the production of maternal milk. It can lead to sexual dysfunction, infertility and menstrual irregularities. Similarly, excess secretion of the hormones FSH and LH rarely results in infertility or menstrual irregularities.
Each of the symptoms related to the pituitary gland is a very good reason to consult a doctor. We have already mentioned that different branches are involved in the examination and tests; for example, neurology and ophthalmology are among them. When the patient has visual disturbances, it should be investigated and the visual field should be examined to see if there is a loss of vision. Or special blood and urine tests should be performed to determine whether there is an increase in the level of hormones in the bloodstream and secreted. If these values are found to be high, tümör can be detected by computed brain tomography or brain-pituitary gland MRI (magnetic resonance).
HOW TO FOLLOW THE PROCESS OF TREATMENT
Tümör küçükse…
When deciding on the treatment method for pituitary tümörürüs, it is important to first look at the clinical findings in the patient and the level of impact on health. In this context, when microadenomas do not cause any functional or anatomical problems, no treatment decision may be made. Close follow-up can be performed in small, non-functional tümös that do not cause any clinical symptoms. In this case, patients will be examined intermittently for any change in the behavior and size of the tümörür. In cases where the symptoms are not too severe and surgery is not required, 70-80% of them can be eliminated with medication. The treatments, which are used to relieve symptoms caused by an increase or decrease in the amount of pituitary hormones in the blood, are especially successful in prolactinomas, which are frequently seen.
Tümör büyükse…
For larger and functional tümörs, different treatment modalities may be required. Surgery may be needed especially for large tumors that cause compression symptoms or pituitary adenomas that are resistant to treatment. Here we can talk about two different methods. The first method, called "endoscopic transnasal transsphenoidal approach", is based on removing the mass with a closed technique using endoscopes inserted into the nose. The second method is to remove the mass by açık neurosurgical method.
Do hormone problems occur after hypophysis surgery?
As we have emphasized, a multidisciplinary approach is important in the follow-up and treatment of pituitary tümörs. When surgery is needed, the experience of the surgical team is another important issue. Successful results are obtained with the hybrid operating room environment and advanced technological devices (such as endoscopic camera systems, nöronavigation, intraoperative MRI) in surgeries performed together with anesthesiologist and otolaryngologist. After the surgery, although very rare, conditions such as pituitary storm due to pituitary hormones being affected, such as pituitary storm and coma may occur. Therefore, the missing hormones should be given to the patient quickly. Conditions such as diabetes insipitus, which we call excessive drinking and excessive urination, can be treated with medication.
Operation and Aftermath…
In surgical treatment, first of all, an area to be used for surgery is created at the back of the nasal pole with the help of an endoscope. After this stage, the tümör is removed. Afterwards, the surgical area is closed with a special tissue preparation. It is also advantageous for the patient to reach the pituitary tümörür through the nose instead of the brain, as long as it is not a large-sized tümör. After this 3-4 hour surgery, there are no stitches and the recovery period is shortened. In navigation-guided surgery, the exact location of the tümörürüis determined, reducing the margin of error and preventing unnecessary injuries.
If there is no serious hormonal imbalance, the patient is discharged within 4-5 days after surgery. However, there are some issues that the patient should pay attention to, especially during the first 7-10 days. Such as not lifting heavy weights or not being constipated. Anything that will increase the intracranial pressure can damage the surgical site and cause a second surgery. It is also important to use tampons for a few days and to follow the scabs well. However, one month after the surgery, patients are completely back to their normal lives. All necessary hormonal follow-ups should also be performed by endocrinology after surgery.
“If the lesion cannot be completely removed by surgery, radiosurgery is a good option. Sometimes this treatment is also used in the presence of lesions or nüks left behind after surgery.”
When RADIOCERRHERY?
Radiosurgery is one of the treatment options for pituitary tümörünüs. With radiosurgery, it is aimed to reduce hormone values to normal levels and to control the growth of the tumor. During radiosurgery, another important goal is to irradiate without damaging the surrounding tissues such as the visual nerve. Tümör is sometimes adhered to the vascular structures on both sides of the nose, making it difficult to remove with surgical methods. Since they are usually benign tumors, there is no need for chemotherapy. However, the treatment is continued with radiosurgery and followed up with MRI examinations. After surgical treatment, stereotactic radiosurgery methods, sometimes using intensified X-rays, can be used to completely clean the area in the event of a growth in the tümör tissue that cannot be removed.